Imagine having a microscopic gatekeeper inside your bloodstream—one that quietly determines your risk for heart disease, yet often goes unnoticed during routine screenings. In the realm of cardiovascular health, that gatekeeper is a key component in cholesterol trafficking and a potent predictor of atherosclerosis. Unpacking its significance reveals not only how fat and lipids travel through your body but also offers actionable insights for more precise cardiovascular risk assessment.
Emerging clinical guidance emphasizes that measuring this protein can be far more informative than traditional cholesterol testing. For instance, evidence shows this marker more accurately reflects the number of harmful lipid particles coursing through your arteries, versus relying solely on LDL-cholesterol numbers, which can hide important variations in particle count and composition PubMed review on apoB. In practice, this means patients with seemingly normal LDL-C levels might still face elevated risk if the particle count is high—information only revealed when this protein is measured.
Clinical guidelines are evolving in response. The National Lipid Association now endorses incorporating this measurement alongside standard lipid panels for a fuller view of cardiovascular risk, particularly in individuals whose traditional metrics don’t align with their true risk profile NLA Expert Consensus. In everyday terms, this means a patient managing metabolic syndrome, obesity, or diabetes might benefit from having this protein measured to fine-tune treatment decisions and monitor therapy effectiveness.
To illustrate, a patient with high triglycerides who appears well-managed by LDL-C standards might still harbor hidden risk due to elevated levels of this protein. Adjusting treatment—possibly by intensifying statin therapy or incorporating lifestyle interventions such as Mediterranean diet adjustments—can meaningfully reduce long-term risk. This personalized approach allows clinicians to catch discrepancies that LDL-cholesterol alone might miss.
This introduction lays the foundation for understanding why this protein plays a pivotal role in precision cardiovascular medicine. In the following sections, we’ll delve into its biology, clinical implications, testing strategies, and real-world applications that empower both clinicians and patients to make smarter, evidence-backed decisions for heart health.
Clinical Insights and Implications
Evidence Linking Elevated Levels to Cardiovascular Outcomes
Recent cohort studies offer compelling evidence that the amount of circulating apolipoprotein B significantly correlates with cardiovascular risk. In an analysis using NHANES data, each standard deviation increase in apoB corresponded with a 13% higher cardiovascular mortality risk, while all-cause mortality demonstrated a U-shaped association, suggesting both excessively high and low levels may carry implications PubMed. Across Scandinavian registry data, individuals with greater “excess apoB” (apoB above that predicted by LDL-C) experienced dose-dependent increases in myocardial infarction and cardiovascular events, reinforcing the added prognostic value beyond traditional lipid measures American College of Cardiology.
Improved Risk Prediction Beyond Conventional Lipids
In the Framingham Offspring Study, accounting for the apoB level beyond expectations from LDL-C or non-HDL-C robustly enhanced prediction models for future coronary heart disease. Including this deviation improved discrimination metrics and model fit, underscoring that particle number—not just cholesterol mass—can be more tightly linked to atherogenesis PubMed. Similarly, in multi-ethnic U.S. cohorts, apoB alone outperformed routine lipid panels in forecasting coronary heart disease mortality, even after adjusting for established risk factors PubMed.
Guideline Perspectives and Clinical Utility
Clinician consensus statements, such as those from the National Lipid Association, advocate combining apoB measurement with standard lipid panels. This dual approach proves particularly useful when lipid values diverge—apoB levels often better reflect cardiovascular risk than LDL-C when discordance occurs. Additionally, apoB assists in characterizing lipoprotein phenotypes and supports cascade screening amid inherited dyslipidemia syndromes—a pivotal tool for personalized preventive strategies PubMed.
Practical Applications and Case Illustrations
Consider a middle-aged individual with moderately elevated LDL-C whose apoB remains disproportionately high despite statin therapy; this scenario may prompt clinicians to intensify therapy or explore adjunctive agents, targeting apoB reduction rather than LDL-C alone. In family screening settings, identifying elevated apoB in close relatives may reveal inherited risk and guide early intervention, long before traditional lipid abnormalities escalate.
Collectively, these findings underscore that evaluating apolipoprotein B offers enhanced insight into atherosclerotic risk, refines individual prognostication, and informs more tailored treatment approaches. In the next portion of our discussion, we’ll explore testing methodologies and interpretation strategies to equip both clinicians and patients with actionable intelligence.
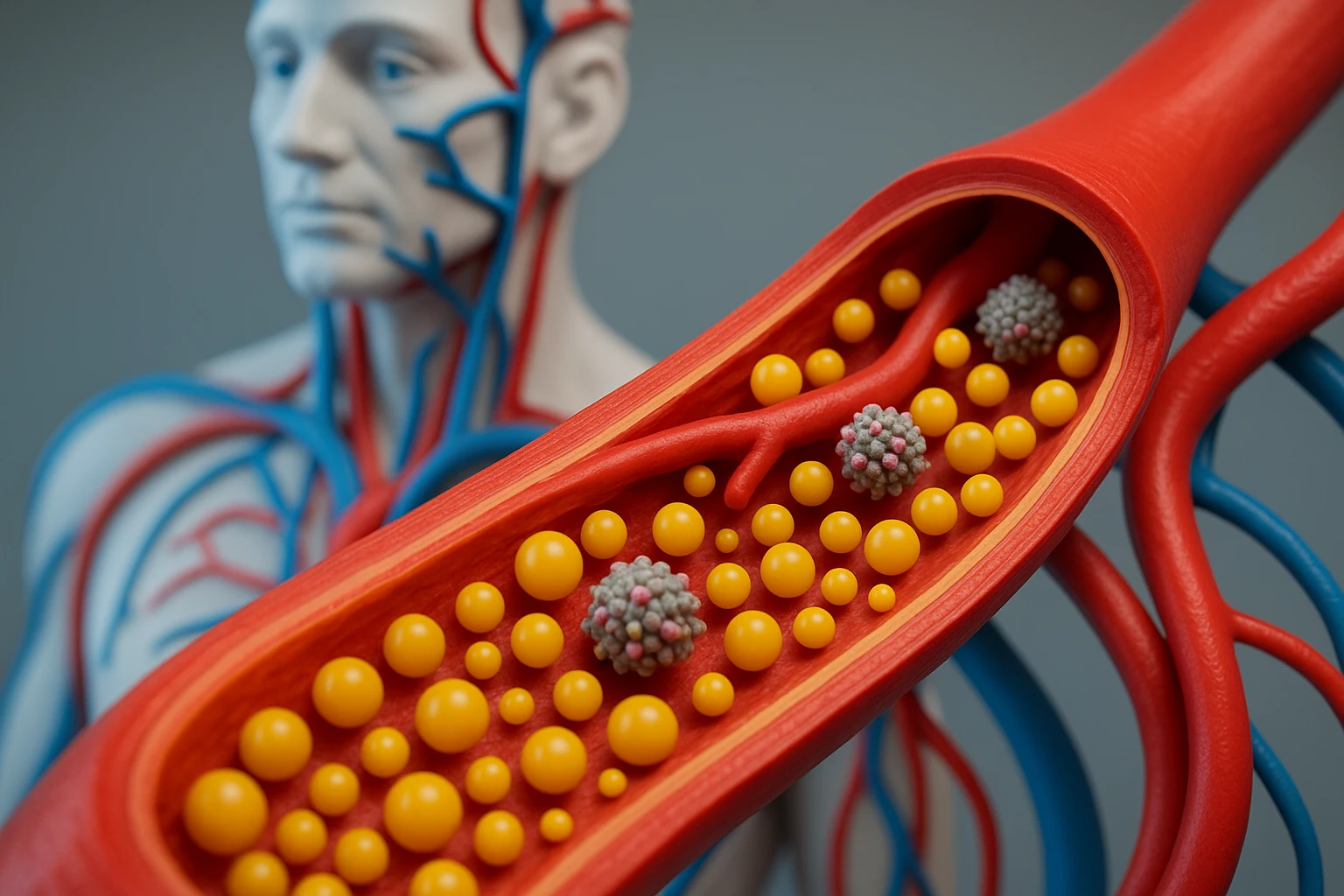
The Role of Apolipoprotein B in Cardiovascular Health
Apolipoprotein B (apoB) plays a crucial role in cardiovascular health, serving as a primary component of low-density lipoprotein (LDL) and very low-density lipoprotein (VLDL). Elevated levels of apoB are often associated with an increased risk of cardiovascular diseases (CVD), as they contribute to the development of atherosclerosis. In fact, many studies suggest that apoB levels can be a more reliable indicator of cardiovascular risk than LDL cholesterol alone.
Understanding ApoB and Lipid Metabolism
ApoB is essential for lipid metabolism, aiding in the transportation and clearance of cholesterol and triglycerides from the bloodstream. It is the main structural protein of LDL particles, each of which contains one molecule of apoB. This makes apoB a valuable marker for assessing the number of atherogenic particles in the blood. According to recent research, individuals with high apoB concentrations have a greater likelihood of developing cardiovascular issues (source).
Clinical Implications and Risk Assessment
Regular monitoring of apoB levels can provide healthcare providers with insights into a patient’s risk for heart disease. Elevated apoB signifies a higher burden of LDL particles, which are directly involved in the formation of artery-clogging plaques. By focusing on apoB rather than just LDL cholesterol, clinicians can make more informed decisions about interventions, such as lifestyle changes or medication.
Innovative platforms like Beek Health offer advanced solutions for monitoring cardiovascular health metrics, integrating seamlessly with healthcare practices to improve patient outcomes.
Case Studies Highlighting ApoB’s Importance
Consider the case of a middle-aged patient with borderline LDL cholesterol levels but significantly elevated apoB. This disparity prompted further investigation and early intervention, potentially averting severe cardiovascular events. In another instance, lifestyle modifications such as diet and exercise effectively reduced apoB levels, supporting the idea that non-pharmaceutical interventions can significantly impact cardiovascular risk (source).
The ability to pinpoint specific lipid irregularities through apoB measurements underscores the importance of personalized healthcare approaches. This precision allows for targeted therapies that address individual risk profiles, ultimately enhancing preventive strategies against heart disease.
Emerging and Targeted Therapeutic Strategies
As researchers continue to seek more precise interventions, innovative therapies targeting lipid components beyond LDL cholesterol are gaining traction. For instance, mipomersen—an antisense oligonucleotide that inhibits the synthesis of apolipoprotein B—has demonstrated significant efficacy in lowering atherogenic lipoproteins across diverse patient populations. In high-risk hypercholesterolemia, mipomersen reduced LDL cholesterol by approximately 36.9%, and apolipoprotein B by 38%, compared to minimal changes with placebo (p < 0.001)⁽source⁾ PubMed study (2013). In those intolerant to statins, reductions reached 47% in LDL-C and 46% in apoB levels⁽source⁾ PubMed study (statin‑intolerant patients). Despite these promising outcomes, treatment was accompanied by notable side effects, including elevated liver enzymes and increased hepatic fat, highlighting the need for careful long-term safety monitoring.
Broader Impact Across Cardiovascular Risk Markers
Beyond inherited hypercholesterolemia, the relevance of apolipoprotein B has been underscored in broader cardiovascular risk prediction. In a large U.S. cohort, baseline apoB levels were found to be better predictors of coronary heart disease (CHD) mortality than traditional lipid measurements—even after adjusting for established risk factors. Specifically, apoB exhibited a hazard ratio near 2.0 for CHD death, outperforming total cholesterol and HDL-C metrics⁽source⁾ PubMed study (atherogenic risk prediction). Similarly, findings from the Framingham Offspring Cohort indicated that apoB improved predictive models beyond LDL-C and non-HDL-C, increasing c‑statistics from 0.72 to 0.73, and enhancing discrimination by up to 11%⁽source⁾ Framingham analysis. Such data affirm the utility of incorporating apolipoprotein B in both prognosis and clinical decision-making.
Translating Evidence into Clinical Practice
Integrating these findings into practice can drive more personalized care strategies. For example, clinicians might consider measuring apolipoprotein B in patients whose LDL-C is deceptively in range yet still experience cardiac events, prompting escalation of therapy. In familial hypercholesterolemia, combining statins with targeted agents like mipomersen may yield marked reductions in residual lipid risk, albeit with vigilance toward hepatic effects. Furthermore, advocating for inclusion of apoB in routine cardiovascular risk assessments could refine treatment intensity decisions, guiding clinicians toward more aggressive lipid-lowering approaches when non-HDL-C or LDL-C readings appear deceptively reassuring.
Altogether, these developments underscore the evolving role of apolipoprotein B—not merely as a marker, but as a therapeutic target that can shape risk stratification and intervention strategies, maximizing clinical benefit while addressing varied patient vulnerabilities.
Conclusion
Understanding the role of apolipoprotein B is crucial in addressing cardiovascular health. As a primary component of low-density lipoproteins (LDL), it acts as a reliable marker for assessing the risk of heart disease. Many studies have demonstrated that elevated levels of apolipoprotein B are linked to an increased likelihood of atherosclerosis, which underscores the importance of this protein in monitoring cardiovascular wellness.
Healthcare professionals should consider incorporating apolipoprotein B testing into routine evaluations for patients who are at risk of heart disease. By doing so, they can implement more targeted prevention strategies and treatments. For instance, lipid-lowering therapies, such as statins, have shown effectiveness in reducing apolipoprotein B levels and subsequently lowering cardiovascular risks. According to research from the NIH, a focus on apolipoprotein B rather than LDL cholesterol alone can enhance treatment outcomes.
For individuals looking to proactively manage their heart health, incorporating lifestyle changes such as a balanced diet, regular physical activity, and weight management can impact apolipoprotein B levels positively. Engaging with these strategies not only improves lipid profiles but also overall well-being.
As we advance in our understanding of lipids and cardiovascular health, staying informed about emerging research and testing methods becomes essential. Utilizing resources and data-driven approaches will empower patients and healthcare providers alike in making informed decisions.
To further explore the implications of apolipoprotein B in clinical settings or for personal health management, consider leveraging expert platforms. Beek Health offers comprehensive resources and professional guidance to navigate these complex aspects effectively. Taking this step can provide valuable support in achieving better cardiovascular health outcomes.
